Biotechnology today has become an incredibly advanced and expansive system of using both biological beings, such as plants or animals, as well as technologies that are constantly evolving the process. The question to put forward now is: how far should biotechnology go to benefit and extend the human lifespan?
In looking through all of the extensive research on the subject, the question can not be easily answered. Both standardized and complex forms of biotechnology (biotech) exist to advance the human’s ability to live a long life, and the larger the gap in between those two is where the ethical grey area lies. And the question then turns to who would be able to enhance their lives employing biotech? In this paper, these questions will largely remain unanswered as biotech continues to advance, change, and become more standardized every year.
Biotechnology
In 1991, the United States’ federal agency the Food and Drug Administration (FDA) defined biotechnology as “the application of biological systems and organisms to technical and industrial processes,” and stated that under this definition the reaction yeast causes in bread-making can be said to be a form of biotech. Yeast is a biological organism that is alive and added to flour to allow the gluten to form larger bubbles, this is a method of biotech that has been used for centuries. Currently, that definition still stands as the backbone of what biotech is, but more specifically, the majority of biotechnology also operates within the realm of molecular science, working on an extremely small level. The University of Kansas defines molecular biotech as “an exciting field fueled by the ability to transfer genetic information between organisms with the goal of understanding important biological processes or creating a useful product” (2018). This is also more commonly known as “recombinant DNA technology or molecular cloning” or gene editing, depending on the exact function and use of the biotech (Glick, et al., 2013).

Forms of gene editing can be dated back for millennia, humans naturally domesticated foods and animals by growing and breeding in specific ways to enhance benefitting features (Avissar, et al., 2019). These benefits can include making corn larger or making animals meatier, all of which are to be advantageous for humans as well as the extension of the human life expectancy: as people are able to survive easier, they are then able to live longer. Push this idea into the modern age, we humans are now able to advance this process down to a molecular level. The company Syngenta has started a movement called the Humanitarian Project in which they transferred the DNA of a daffodil into a rice plant in order to create what they call “Golden Rice” (Paine, et al., 2005). “Golden Rice” is a working prototype of the company’s goal: to donate vitamin A-rich rice to areas in the world that are deficient in the vitamin, which can lead to other health concerns (Paine, et al., 2005). Biotechnology expansions like this can be used to advance the human lifespan in less developed or lower-income areas.
Outside of agricultural progression, there are also medical advancements that have aided in humans living longer. “Recombinant DNA technology was used to produce large-scale quantities of the human hormone insulin in E coli. as early as 1978 … to treat diabetes,” more recent examples of common biotech in medicine include vaccinations, antibiotics, and hormones “to treat growth disorders in children” (Avissar, et al., 2019). Using inactivated clones of viruses, scientists can produce vaccinations that can fight continually developing strains of that same virus (Avissar, et al., 2019). These examples show ways in which scientists have been able to create what we know today as “modern medicine” using biotech. Over the past 200 years, throughout all medical strides, the worldwide average life expectancy has gone from roughly 30 years of age to nearly 80 years (Roser, Ortiz-Ospina, Ritchie, 2019), and this could largely be because of biotechnology developments like vaccinations and antibiotics.
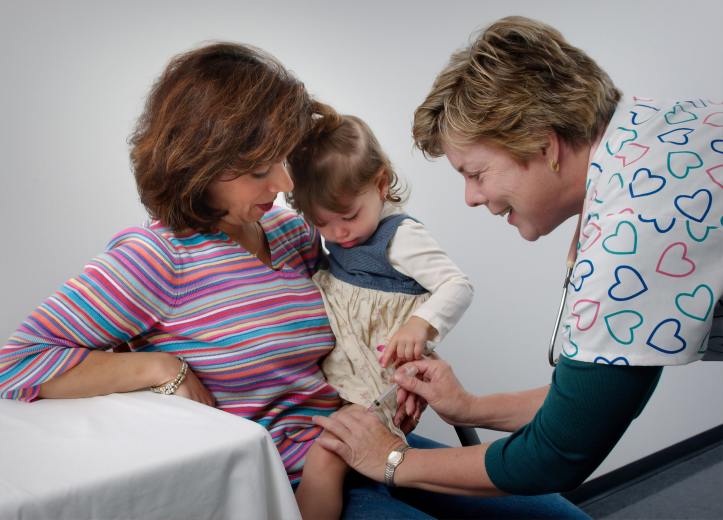
The ethical aspect involves the use of biotech in changing the DNA patterns of human beings. Another form of gene editing is gene therapy, this consists of two different types. The first is germline gene therapy, which is used to treat hereditary disorders within fertilized eggs (Glick, et al., 2013). Germline gene therapy is the type of biotech that can potentially be used to create what is known as “designer babies” – it could also be used to eliminate unwanted features and for this reason is dubbed questionably unethical. Who is it to say what is a serious condition to be removed ought to be, or are they more leaning toward simply unwanted features? The second type is somatic cell gene therapy, which is used on non-germline cells and is also broken down into two parts: introducing new genes into either stem cells or other organs and tissues to treat disorders (Glick, et al., 2013).
Stem cells are similarly divided into two parts: embryonic and somatic, and these can be found in embryos, umbilical cords, blood, and bone marrow (Glick, et al., 2013). The FDA currently sets high regulations on the stem cell use and research and says that “there are a small number of unscrupulous actors who [are] exploiting the uncertainty, in order to make deceptive, and sometimes corrupt, assurances to patients based on unproven and, in some cases, dangerously dubious products … In addition, the FDA will continue to work closely with industry to find other ways to aid in the effort to bring novel therapies to patients” (Office of the Commissioner & Gottlieb, 2018). More recently, the FDA began investigation processes on said actors who were putting both the umbilical cord donors as well as the product consumers/patients at risk – because cord blood is difficult to store, the company could have had contaminations such as “viruses or microorganisms or have other serious product quality defects” (Office of the Commissioner, 2019). It is for reasons like this that research and development on biotechnology ought to be handled extremely carefully.
The Human Lifespan
Apart from “dubious actors” in the medical market, an additional reason why biotech is an ethically grey area is the public’s reaction to the prices of such healthful advancements. As mentioned, the global average lifespan has gone from 30 years to 80 years of age (Roser, Ortiz-Ospina, Ritchie, 2019), but that statistic does not properly paint a picture of what that average makes up. Setting two maps side-by-side, one reporting the average lifespan by country and the other the average household income, one can see just how off-setting on average an annual income can do to one’s overall health.
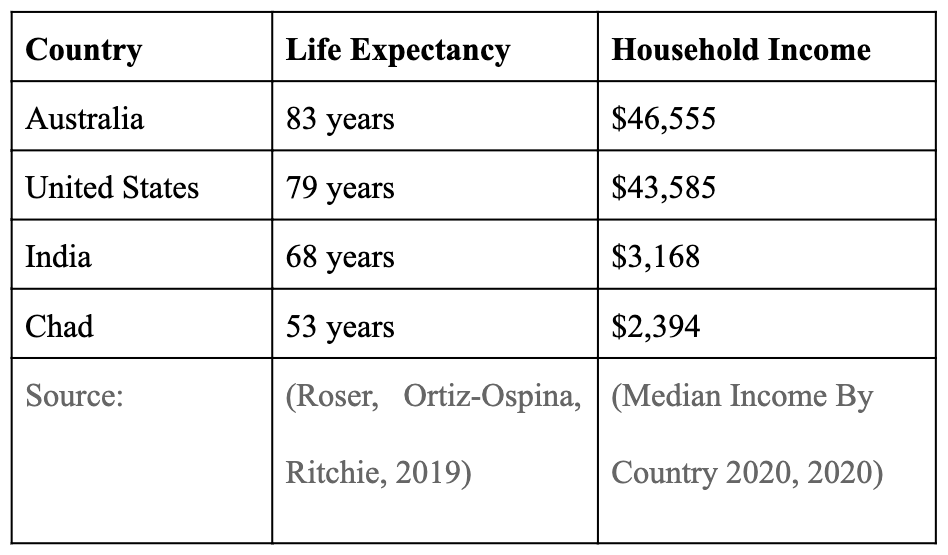
Shown here is a graphic with four example countries (Australia, United States, India, and Chad), all with various life expectancies, with a 30-year and $44,000 difference between the highest and lowest.
In addition to this, a smaller-scale study on the same relationship found that “most of the variation in life expectancy across geographic areas was related to differences in health behaviors, including smoking, obesity, and exercise” (Chetty, et al., 2016). There are many variables to consider in wanting to extend the overall human lifespan, and one of the most important ones would be this: who can afford an extended lifespan? Who currently can afford modern medicine as it is today?
With a current life expectancy difference of 30 years across different countries, and “modern medicine” to be thankful for – more ethical decisions lie in extending the lives of the already fortunate population who can afford such extremities. Especially considering that 30 years this is the same number between medically advanced countries now and 200 years ago.
Biotechnology in Effect
The company Novartis’ new treatment called Kymriah was the first FDA approved form of somatic gene therapy, which was developed to help those with B-cell acute lymphoblastic leukemia (commonly called ALL) and is reserved for the 15-20% of patients “whose cancer has not responded to” previous alternative treatments (Office of the Commissioner, 2017). In Novartis’ initial clinical trial, 83% of the 63 patients were in remission after a median average time of 29 days (Novartis, 2018). But Kymriah also carries serious to fatal side effects as well, patients have died from this in other clinical trials from cerebral edema, “a condition in which excessive fluid causes the brain to swell” (Ramsey, 2017). In an interview with the president of Patients for Affordable Drugs, David Mitchell shared with Forbes magazine that “Novartis’ $475,000 breakthrough should cost just $160,000” for the consumer/patient (Herper, 2018).
In a 2000 cost analysis on treating the same form of cancer, “total mean cost of the entire treatment was US $103,250 per patient, 53% of which were basic hospital costs” and the rest in “laboratory tests and radiology,” specific inhibitor medications, and “blood products” (Rahiala, et al., 2000). While this analysis is 20 years old, this break down is nearly an exact fifth of Novartis’ price for their Kymriah drug therapy and follows more closely with Mitchell’s assessment. Moreover, the cost analysis study also stated that “80% of children with ALL are long-term survivors” (Rahiala, et al., 2000), which is a 3% difference of remission from utilizing Kymriah. This is just one of many examples where a medical treatment that could be extremely beneficial, towards one’s life expectancy and advancing the global human lifespan, is widely unavailable to the general public because of its price.
Another instance of gene therapy is by the company Spark, who set out to make advancement towards a disease without any other alternative treatments. “Before Luxturna, there were no available cures for any of the inherited retinal diseases. The most that doctors could do was offer visual aids for those with retinal dystrophies,” but as children age, their vision only grows worse (Gingerich, 2019). “Children have been successfully treated for inherited vision loss at the University of Michigan’s Kellogg Eye Center. Luxturna, the first therapy to treat this disease, was approved by the FDA in late 2017” (Gingerich, 2019). This sort of germline gene therapy was also the first of its kind to be approved as it attacks a disorder that is hereditary. We can expect to see longitudinal studies in the future for Luxturna and drugs like it as they come onto the market to see if the children of these patients pass down their removed inherited disorders, or if the treatment only cures the prescribed generation.
Outside of this new question, the company did address the fiscal ethical issue: “Many analysts expected Spark’s drug might be priced at $1 million – and Spark’s chief executive, Jeffrey Marrazzo, said … the drug could support a value in excess of that sum. [They] chose a lower price: $425,000 per eye, because insurers indicated that pricing the drug higher would trigger restrictions on which patients could get access” (Johnson, 2018). An ophthalmologist who treats young children at the Kellogg Eye Center says that “ultimately, we want these therapies to be available for our youngest patients. The sooner they receive treatment, the less vision loss they may have to endure” (Kirkendoll, 2019). It can be appreciated that the company had the consumer/patient in mind when setting the price, medical advancements ought to be as available as they are made to be beneficial, and for this disorder, it is parents and their insurance who are footing the bill. So with a large heart, Spark made its price $150,000 less than the market’s expectations and with insurance brackets in mind.
Discussion
While thinking about the price of all of the time, the research, patenting, and all of the other steps that creating a new drug takes, the company ought not to see a profit as the end goal as much as they should see a worldwide improvement on human health just as Spark’s company has shown. As well as Syngenta, with their Humanitarian Project and wanted to enriched less fortunate areas with vitamin A-enhanced, daffodil-infused Golden Rice. Working towards a larger goal like this, to extend the human lifespan and overall quality of life, is the most ethical route to advancing biotechnology.

Biotechnology is a sizable area with a lot of complex details, but more largely, biotech is neither black nor white and this is why the FDA is constantly moving toward benefiting the public through innovation and constant vigilance. Common medicines like vaccinations, antibiotics, insulin, and hormones have been standardized to help all people in all socioeconomic classes as most are covered by even the freest of insurances – these too are steps toward an ethical medical future, where there is a means for even the lowest of income families to have the same access to the same medicines as those in higher-income classes. And with a roughly 30-year difference in life expectancy between the most advanced countries against the least being the same as if it were against the same country 200 years ago, there ought to be more priorities set to where extended lifespans are available.
While there may be complex terminal diseases today that we could study further, there are still countries out there that are in need of already developed medicines, or possibly new products as shown by the company Syngenta. This is not to mention all of the employment and financial entanglement that would occur if people in the United States were to grow up to be 100 years of age on average, as well as the swoll of the robotic industry taking over. One question may then lie in this: should we extend the human lifespan any further than what it is today? Opening the doors up to germline gene editing could risk the population to become overabundant and then this would off-set the world’s population past the point of which it can carry far too quickly than we would be able to sustain proper life. Ultimately ending in a shorter lifespan than scientists originally intended.
More and more questions could be answered on the very same topic of utilizing medical advancements to our own benefit. For instance, prenatal genetic screening on babies, ultimately the first step toward germline gene editing where parents are picking and choosing their baby’s DNA sequence. Or the new-found knowledge of a baby having a terminal disease, or a disease that may give them a harder life than others, these sort of circumstances lead parents to have to make large life decisions. And if prenatal genetic screening were standardized or normalized, then there could be a potential for the human life expectancy to be altered by a changed ratio in the population on who has genetic disorders that lead to earlier deaths and who does not.
These questions found throughout this paper can lead to larger works in ethical research and discussion. To the original question: Is it ethical to use the advances in biotechnology to extend the human lifespan? Only if the means to do so are standardized to a point in which all socioeconomic classes have the technology available to them, moreover, biotech innovations ought to be pointed toward more diseases with no other alternative cure to this date, as the company Spark’s ingenuity exemplified with their work in extinguishing hereditary vision loss.
References:
Avissar, Y., Jurukovski, V., Fowler, S., Wise, R., Roush, R., Choi, J., … Gair, J. (2019, May 1). 10.2 Biotechnology in Medicine and Agriculture. Retrieved February 24, 2020, from https://opentextbc.ca/biology/chapter/10-2-biotechnology-in-medicine-and-agriculture/
Chetty, R., Stepner, M., Abraham, S., Lin, S., Scuderi, B., Turner, N., … Cutler, D. (2016, April 26). The Association Between Income and Life Expectancy in the United States, 2001-2014. Retrieved April 8, 2020, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4866586/
Gingerich, C. P. (2019, March 30). Luxturna Successfully Used to Treat Inherited Retinal Disease. Retrieved April 8, 2020, from https://www.mdmag.com/medical-news/luxturna-treat-inherited-retinal-disease
Glick, B. R., et al., (2013). Medical Biotechnology, ASM Press. Retrieved February 24, 2020, from http://ebookcentral.proquest.com/lib/gvsu/detail.action?docID=1747238.
Herper, M. (2018, February 8). Patient Advocate Says Novartis’ $475,000 Breakthrough Should Cost Just $160,000. Retrieved April 8, 2020, from https://www.forbes.com/sites/matthewherper/2018/02/08/patient-advocate-says-novartis-475000-breakthrough-should-cost-just-160000/#4863a5d35152
Johnson, C. Y. (2018, January 3). Gene therapy for inherited blindness sets precedent: $850,000 price tag. Washington Post. Retrieved April 8, 2020, from https://link-gale-com.ezproxy.gvsu.edu/apps/doc/A521219983/OVIC?u=lom_gvalleysu&sid=OVIC&xid=d20346bf
Kirkendoll, S. M. (2019, February 7). Gene Therapy Treatment Targets Rare Mutation Tied to Blindness. Retrieved April 8, 2020, from https://labblog.uofmhealth.org/health-tech/gene-therapy-treatment-targets-rare-mutation-tied-to-blindness
Median Income By Country 2020. (2020, February 17). Retrieved April 9, 2020, from https://worldpopulationreview.com/countries/median-income-by-country/
Novartis. (2018). Highlights Of Prescribing Information. East Hanover, NJ: Novartis Pharmaceuticals Corporation. Retrieved April 8, 2020, from https://www.fda.gov/files/vaccines%2C%20blood%20%26%20biologics/published/Package-Insert—KYMRIAH.pdf
Paine, Jacqueline A, et al., (2005). Improving the nutritional value of Golden Rice through increased pro-vitamin A content. Nature Biotechnology, vol. 23, no. 4, p. 482+. Accessed April 9 2020, from https://link-gale-com.ezproxy.gvsu.edu/apps/doc/A190565916/OVIC?u=lom_gvalleysu&sid=OVIC&xid=ee6cfd9e.
Rahiala, J., Riikonen, P., Kekäläinen, L., & Perkkiö, M. (2000, April). Cost analysis of the treatment of acute childhood lymphocytic leukemia according to Nordic protocols. Retrieved April 10, 2020, from https://www.ncbi.nlm.nih.gov/pubmed/10830464
Ramsey, L. (2017, August 31). A medical breakthrough that hacks genes to fight cancer just got approved, and it’s the beginning of ‘a big new field of medicine’. Retrieved April 8, 2020, from https://www.businessinsider.com/why-the-fda-approved-kymriah-a-car-t-cell-therapy-to-treat-cancer-2017-8
Roser, M., Ortiz-Ospina, E., & Ritchie, H. (2019, May 23). Life Expectancy. Retrieved April 9, 2020, from https://ourworldindata.org/life-expectancy
Office of the Commissioner. (2019, September 3). FDA sends warning to company for selling unapproved umbilical cord blood and umbilical cord products that may put patients at risk; continues to warn patients of the risk of unapproved stem cell therapy. Retrieved April 9, 2020, from https://www.fda.gov/news-events/press-announcements/fda-sends-warning-company-selling-unapproved-umbilical-cord-blood-and-umbilical-cord-products-may
Office of the Commissioner, & Gottlieb, S. (2018, March 27). Statement from FDA Commissioner Scott Gottlieb, M.D. on the FDA’s new policy steps and enforcement efforts to ensure proper oversight of stem cell therapies and regenerative medicine. Retrieved April 8, 2020, from https://www.fda.gov/news-events/press-announcements/statement-fda-commissioner-scott-gottlieb-md-fdas-new-policy-steps-and-enforcement-efforts-ensure
Office of the Commissioner. (2017, August 30). FDA approval brings first gene therapy to the United States. Retrieved April 8, 2020, from https://www.fda.gov/news-events/press-announcements/fda-approval-brings-first-gene-therapy-united-states
Office of Regulatory Affairs. (1991, November). Biotechnology Inspection Guide (11/91). Retrieved April 9, 2020, from https://www.fda.gov/biotechnology-inspection-guide-1191
The University of Kansas. (2018, October 26). What is Molecular Biotechnology? Retrieved April 9, 2020, from http://www.kumc.edu/school-of-health-professions/clinical-laboratory-sciences/masters-in-molecular-biotechnology/what-is-molecular-biotechnology.html
